Facts about morphine and other opioid medicines in palliative care
Facts about morphine and other opioid medicines in palliative care
Friday, February 05, 2021
What is this brochure about?
Opioid medicines are pain relievers. They include medicines such as codeine, morphine and oxycodone. Knowing the facts and helping to unravel a few myths, will help you and your carers understand opioid medicines and therefore manage your pain effectively so you can get on with living as well as possible with your life-limiting illness.
Facts about morphine and other opioid medicines for pain in palliative care_ February 2021
(updated February 2021)
What is palliative care?
Palliative care is an approach designed to improve quality of life for someone living with a life-limiting condition. It focuses on your needs, as well as those of your family and carers, and it can begin as soon as you have been diagnosed. Managing your pain is an important part of palliative care.
What is pain?
Pain is an unpleasant sensation, suffering or distress. All pain hurts and can wear you down. Pain can make you irritable, make it hard to sleep, reduce your appetite, and make it hard to be active and enjoy life.
Facts about pain
- Not everyone with a terminal illness will experience pain.
- Everyone experiences pain differently, so the way you experience pain will be unique to you.
- Most pain can be relieved to a level that allows you to continue to live your life.
- Pain can be due to different reasons dependant on the cause and therefore it may take more than one type of analgesia to control it.
- Pain is not always constant, it can change over the day and with different activities and can fluctuate with your moods, emotions and family life.
Managing your pain is an important part of palliative care
Assessment of your pain
The conversation
Pain management starts with having a conversation with your health care professional, whether that be your GP, your specialist such as an oncologist or respiratory physician, or your palliative care team. It is essential that you are open and honest about your pain so it can be assessed and planned for, for you as an individual.
Facts about your pain that your health care professional needs to know
To get a clear picture of your pain, your doctors and nurses will ask the following questions; (based on SOCRATES mnemonic acronym often used in pain assessment)
- Site – Where is the pain?
- Onset – When did the pain start? Was it sudden or gradual? Is it getting worse or better?
- Character – What is the pain like? Stabbing? Dull? Crushing? Burning? etc
- Radiation – Does the pain radiate anywhere?
- Associations – Any other symptoms associated with the pain?
- Time course – Does the pain follow any pattern?
- Exacerbating/relieving factors – Does anything make the pain worse or better
- Severity – How bad is the pain? (Pain scale 0-10 is often used or Abbey pain scale or Wong-Baker FACES® such as the adaption below)
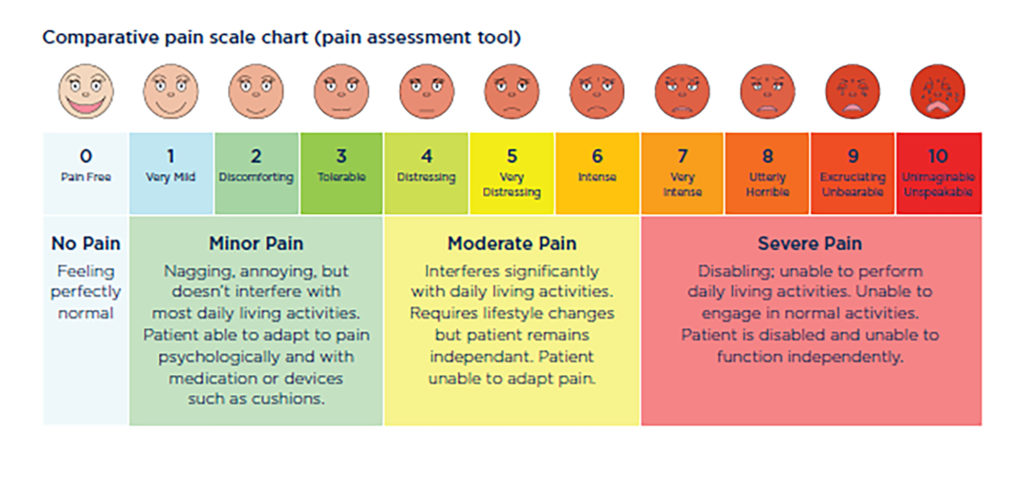
Comparative pain scale chart (pain assessment tool)
Non-Pharmacological Pain Management
Non-pharmacological ways in which to relieve your pain may be explored first such as heat packs, positioning, physiotherapy, alternative therapies etc. It may be that you have tried things yourself, it is helpful to communicate about whether or not these things have helped you to better direct the pain management plan.
It’s important to tell your doctor about all the medicines you are taking, including any over-the-counter, herbal and natural medicines, so you aren’t unintentionally prescribed a medicine that you are already taking or one that interacts with your current medicines.
Pharmacological Pain Management
Opioids
Opioids are medicines that are prescribed for strong or severe pain that is no longer responding to medications of lesser strength. They come in different formulations such as tablets, patches or a liquid and your prescriber will discuss which one is best for you and your individual pain treatment. They have also been found to be effective in managing shortness of breath and it may be that you are prescribed an opioid for pain and/or shortness of breath management. Opioids also have a role in managing severe diarrhoea and cough.
Intermittent (or ‘as needed’) dosing
Your medical or nurse practitioner will most likely start you on an intermittent regime of an opioid to take as you need it within certain time parameters. You will need to keep a record of when you take the medication and its effect on your pain and any other side effects, so you can show this to your practitioner at your review. It is essential that you contact them if you have any unwanted side effects to discuss as quickly as possible so an alternative can be sought for you. Also your community pharmacist is an important resource in medication management and you may want to discuss the medication with them as well.
Slow release dosing
Once you have a documented regime that shows you would benefit from a slow release opioid, your practitioner will provide you with a new regime.
This slow release tablet may be taken once or twice a day or you may have a patch that needs to be changed every 3 or 7 days, dependent on your clinical need. You will still be able to take intermittent dosing as pain can still be a problem with your daily activities and it is essential that you can control it so you can continue living well with your disease. It is very important that if you are needing more than 3 intermittent doses per day, that you contact your practitioner to revisit your slow release dose. Also remember that this type of medication cannot be crushed or broken into smaller parts.
Combination dosing
Your practitioner may prescribe other medications such as a weak analgesia like paracetamol which can complement opioid management or an adjuvant. Adjuvants help with other types of pain such as neuropathic (nerve) or visceral (organ), and can provide an umbrella effect with addressing all aspects of your individual experience of the pain. Often adjuvants can help reduce the need to increase opioids and can provide a more steady state in your pain management experience.
Opioids are prescribed for strong or server pain that is no longer responding to medications of lesser strength
Medicine names
All medicines have two names: a generic name and a brand name. Each medicine has only one generic name, but if it is sold by more than one company it will have different brand names. For example, the generic name is oxycodone and its trade name for the long acting formulation is Oxycontin and the short acting 5mg tablet is Endone and all doses 10mg and up are called Oxynorm.
Ask questions
If you have any questions, ask them. There’s no such thing as a stupid question: all your questions are good questions. Write down your questions beforehand or when you think of them, and make sure you get the answers you need.
Take as prescribed
Take your medicines regularly at the times prescribed (or as close as possible to those times) to get the maximum benefit from them. For example, delaying an opioid medicine that takes time to start working may result in you experiencing pain that could have been avoided.
Learn about and organise your medicines
Knowing when, how and why to use your opioid medicines, and knowing who to ask if you have problems is a big part of achieving good pain relief. If you have any questions about your medicines, ask your prescribing practitioner or another member of your health care team which includes your pharmacist.
Organising your medicines safely and having an adequate supply on hand so you never run out, particularly over weekends or public holiday, is also essential. Ask your pharmacist for advice, and talk to them about packaging your medicines in a weekly medication organiser and about safe storage.
Cost of your medicines
Most opioid medicines are supplied under the Pharmaceutical Benefits Scheme (PBS), so their cost is subsidised by the Australian Government. If you are having difficulty paying for your medicines, talk to your practitioner so they can prescribe medicines you can afford. Also, talk to your pharmacist about ways to save money on your medicines.
Facts about using opioid medicines
Using opioid medicines appropriately involves:
- storing your medicines at the correct temperature and out of reach of children
- measuring your doses carefully and accurately
- knowing when it’s okay to crush and split tablets, and mix them with other substances
- setting up reminders to help you to take your medicines on time
- recording when you’ve taken your medicines
- recording the effects of your medicines, especially any side effects or unusual reactions, and telling your doctor about them as soon as possible
- knowing what to do if you forget or miss a dose – for example, whether you take it when you remember or wait until the next scheduled dose?
- knowing whether you can drink alcohol – small amounts of alcohol are usually okay, but alcohol may make you more drowsy
- knowing whether you can drive or use machinery
- not intentionally missing or changing your medicines without telling your medical or nurse practitioner
- disposing of unused medicines by returning them to your pharmacist
Myth busting Opioid Medications
There are many myths about opioid medicines. Knowing the facts and busting the myths will help you use your opioid medicines wisely.
Morphine and other opioid medicines hasten death
Some people fear that being prescribed opioid medicines means that they’re closer to the end. Relieving your pain changes your quality of your life, not its length.
Opioids have side effects
Sometimes people worry that the side effects of their opioid medicines will be worse than their pain. Not everybody experiences side effects and it is important to remember that side effects are not an allergic reaction, and are often temporary and manageable.
Common possible side effects of opioid medicines include:
- Constipation: can be relieved by taking laxatives
- Nausea and vomiting: often temporary and can be relieved with anti-emetic medication
- Drowsiness or confusion: may occur for only a short time after starting treatment or increasing the dose
- Dry mouth: may improve with time, speak to your pharmacist for help if this occurs
Tell your doctor promptly about any side effects, their severity and when they occur. Your doctor may be able to alleviate them by changing the dose or the medicine.
Relieving your pain improves your quality of life, not the length of your life
Opioid medicines mask you knowing how your illness is progressing
Some people stop taking their pain medicines because they are worried the medicines will mask the progression of their illness so they won’t know how they are really feeling. Pain medicines will not stop your health care team or you from monitoring the progress of your illness because there are other signs and symptoms of progression that will be present.
Pain management shouldn’t start until the pain is unbearable
Some people only tell their doctor about their pain when it gets really bad. However, it is usually easier to manage pain in its early stages and that provides a good start to ongoing management requirements and gives the practitioner historical information about your pain.
Breakthrough pain means the plan isn’t working
Breakthrough pain is pain that occurs while on slow release pain management. This is a normal part of living with your illness and you may find that your pain occurs at predictable times of the day ie having a shower, going out in the car, in the earlier hours of the morning. Your practitioner will provide you with a suitable medication for intermittent dosing that you can use pre-emptively or at the time of the pain occurring. It is essential you keep a diary of this use to be reviewed by your practitioner to make sure your plan is still meeting your needs as an individual.
References
- Vagg, M., 2015 The right words matter when talking about pain. The Conversation. www.theconversation.com/the-right-words-matter-when-talking-about-pain-50450
- Australian Adult Cancer Pain Management Working Group, 2016. Cancer pain management in adults- screening. https://wiki.cancer.org.au/australia/Guidelines:Cancer_pain_management/Screening#References
- Comparative Pain Scale Chart., www.123rf.com/photo_61431492_stock-vector-faces-pain-scale-doctors-pain-assessment-scale-comparative-pain-scale-chart-faces-pain-rating-tool-v.html Cited August 2018
- CareSearch., 2017 Non Pharmacological Approaches www.caresearch.com.au/caresearch/tabid/751/Default.aspx
- World Health Organisation, cited August 2018 http://www.who.int/cancer/palliative/painladder/en/
- CareSearch., 2017 Myths About Morphine https://www.caresearch.com.au/caresearch/tabid/2400/Default.aspx
Additional resources used
HammondCare., 2014 Pain Management in Palliative Care http://www.palliativecarebridge.com.au/resources/PainManagementInPalliativeCare.pdf
The Pharmaceutical Benefits Scheme., 12th July 2018 About the PBS http://www.pbs.gov.au/info/about-the-pbs
Want more information?
Your best source of information is your doctor and care team.
There may be times when you want additional information from one of the many organisations that provide help to patients and their families.
Palliative care
Palliative Care Australia Inc. (PCA) can direct you to your state or territory palliative care association. The PCA website also has useful information about palliative care, a directory of palliative care services, and other resources for patients and carers.
T 02 6232 0700 (office hours)
W Palliative Care Australia
Medicines
The pharmacists at Medicines Line can answer your questions about medicines for the cost of a local call. Remember to tell them that your medicines are being prescribed for palliation.
T 1300 633 424 (office hours)
Caring for a person with palliative care needs
Commonwealth Carer Resource Centres have services and information for family carers.
T 1800 242 636
W www.carersaustralia.com.au
YOU CAN FIND MORE SUPPORT INFORMATION AND RESOURCES LIKE THIS ON OUR WEBSITE
Disclaimer: PCA advises the information in this brochure is not clinical advice. Your health care decisions are best made in consultation with your practitioner. PCA provides these links for information purpose only. It is not responsible for the content of these websites.
Updated February 2021
Palliative Care Australia ABN 85 363 187 904
P: 02 6232 0700
E: pca@palliativecare.org.au
palliativecare.org.au
Download - Facts about morphine and other opioid medicines in palliative care (updated February 2021)
Download - PCA's Position Statement: Sustainable access to prescription opioids for use in palliative care